Pathogenesis, diagnosis and management of thyroid nodules in children
-
Figure 1
A possible diagnostic work-up in palpable thyroid nodules.1Control visit after 4 weeks (clinical examination plus ultrasound; FNAB – if indicated by, for example, palpable solid remnants of the cyst or peripherally localized solid tissue within the cystic lesion). 2Next visit after 6–8 weeks and then a 3 month interval (supplementary l-T4 therapy if indicated; surgery if relapse). 3Higher risk of malignancy in nonclassic subtype. 4Consider molecular markers: if positive–surgery, if negative–surgery in cold and hot nodules vs follow-up in a warm nodule. 5Next visit after 4–6 weeks and then a 3 month interval (l-T4 – if indicated and consider FNAB or direct surgery if tumor enlargement or suspicious appearance on US). 6Any palpable solid/or mixed, cold/or hot nodule should be removed even with benign cytology but the time and the extent of surgery may differ, depending on all the diagnostic data.
-
Figure 2
Ultrasound imaging of selected forms of thyroid nodular disease. (A) Nodule in congenital hypothyroidism (solid hyperechogenic vs hypoechogenic extranodular area after l-T4 withdrawal for 2 weeks). (B) Hemiagenesis of thyroid (enlarged right lobe with a small mixed lesion). (C) Hyalinizing thyroglossal duct cyst localized outside thyroid. (D) Cystic nodule (unechogenic lesion). (E) Familial multinodular goiter (solid isoechogenic lesions). (F) Oxyphilic follicular adenoma (solid hypoechogenic lesion). (G) Atypical follicular adenoma (solid hypoechogenic lesion). (H) Papillary thyroid carcinoma coexisting with Graves’ disease (solid hyperechogenic lesion vs hypoechogenic thyroid). (I) Papillary thyroid carcinoma coexisting with autoimmune Hashimoto thyroiditis (solid hyperechogenic lesion vs hypoechogenic thyroid). (J) Papillary thyroid carcinoma coexisting with autoimmune Hashimoto thyroiditis (solid hypoechogenic lesion within the less hypoechogenically remaining part of thyroid).
-
Figure 3
Ultrasonographic dynamics in the course of a benign non-neoplastic lesion (hemorrhagic cyst). From appearance (A) via hematoma post-FNAB (B), hematoma on Doppler (type I vascularization – lack of intranodular vascular network) (C), to almost complete resorption within 6 weeks (D). Longitudinal projection (from Niedziela 2002).
-
Figure 4
Ultrasound imaging of thyroid carcinoma. (A) Papillary thyroid carcinoma (solitary solid hypoechogenic lesion with irregular borders; tumor not detected on palpation). (B) Oxyphilic follicular thyroid carcinoma (solid hypoechogenic lesion with irregular borders). (C) Follicular variant of papillary thyroid carcinoma (hypo/isoechogenic pattern of the lesion). (D) Papillary thyroid carcinoma (multifocal form). (E) Papillary thyroid carcinoma with microcalcifications. (F) Follicular thyroid carcinoma (cold on scintigraphy) with a high intranodular flow with Doppler (type III vascularization – increased perinodular and intranodular). (G) Local lymph node metastases. (H) Follicular adenoma (classic hot nodule with a high vascular flow with Doppler and no visible flow in the remaining part of the thyroid.
-
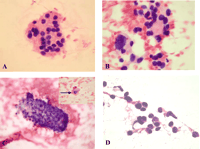
Figure 6
Cytological picture of selected forms of thyroid nodular disease in children suspected of neoplasia, either benign or malignant (H&E staining). (A) Follicular lesion. (B) Suspicious result. (C) Papillary thyroid carcinoma (one papilla and a single cell with intranuclear vacuole). (D) Medullary thyroid carcinoma.
- © 2006 Society for Endocrinology